ScienceDaily (Mar. 23, 2011) — The latest clues suggesting potential new ways to treat melanoma come from an unlikely source: fish.
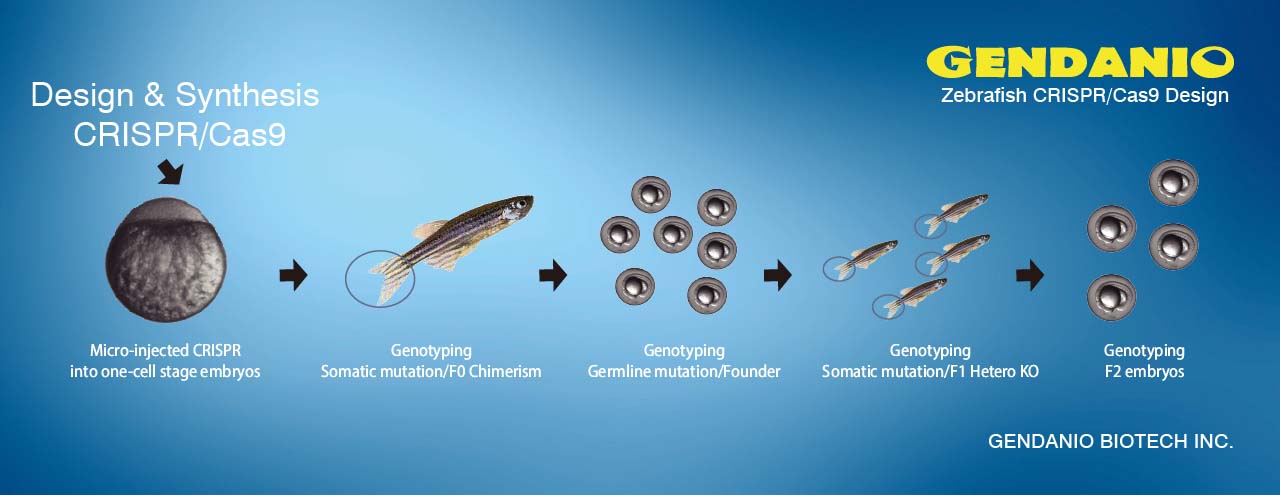
Zebrafish don't get sunburns, but they can get skin cancer -- at least those fish that have been engineered to model the often deadly human cancer. When Leonard Zon, a Howard Hughes Medical Institute investigator at Children's Hospital Boston, developed this melanoma model five years ago, he hoped to use the tiny striped fish to discover new melanoma genes or new therapies for this aggressive cancer that consistently eludes treatment.
Now, in work described in two papers appearing in the March 24, 2011, issue of the journal Nature, he has done both. Zon and colleagues at multiple institutions used the zebrafish model to discover two new melanoma-promoting proteins that could be targets for therapy. The first, SETDB1, is an enzyme that controls the activity of other genes. It was never suspected of playing a role in cancer, but the new studies show that too much of it can accelerate melanoma.
In a second set of experiments, a team led by Zon examined zebrafish embryos and found that shutting down a protein involved in converting DNA to RNA can block the formation of stem cells that give rise to melanoma. Encouragingly, this can be achieved with an existing arthritis drug. The research also demonstrated this drug works additively with another drug now being evaluated in clinical trials for metastatic melanoma, suggesting that this combination may be a viable option for treating human melanoma.
Melanoma, though still relatively rare, is on the rise in the United States, accounting for 68,000 new cases and 8,700 deaths in 2009. The quest to conquer melanoma begins with trying to understand what turns pigmented cells called melanocytes malicious. In 2002, researchers discovered that about 80 percent of human melanomas have a mutation in the BRAF gene that drives proliferation of the melanocytes. Zon put that gene into zebrafish that also lacked the tumor suppressor gene p53. This made the melanocytes that normally fashion the fish's stripes become darker, splotchy and often cancerous. But benign moles can also have the BRAF mutation, so while it may initiate the process, other genes or pathways must conspire to cause melanoma.
In the first Nature paper, Zon and his 21 coauthors looked for those other genes in a region on human chromosome 1, and found 17 genes that were amplified, or duplicated, in melanoma samples. Having extra copies of a gene can cause cells to overproduce the protein it encodes. When the protein is one that promotes cell growth, too much of it can trigger cancer.
To see if any of the duplicated genes they found accelerated melanoma in zebrafish, Craig Ceol and Yariv Houvras, postdoctoral researchers in Zon's lab, created a handy genetic vehicle, the MiniCoopR, that carried the 17 human genes one-by-one into melanoma-prone zebrafish.
Using "brute force" to analyze more than 2,100 tumors in 3,000-plus fish, the researchers found just one gene, SETDB1, that accelerated melanoma. It made the cancer appear earlier, grow faster, and invade deeper into the muscle and spine. By screening 100 human melanoma cell lines, the team found that SETDB1 was also up-regulated in 70 percent of the tumors.
Extensive biochemicial analysis showed that SETDB1 produces an enzyme that regulates gene expression epigenetically, by modifying the DNA-bearing chromatin in the structure of the chromosome. "What's nice is that enzymes can be inhibited and that could lead to new therapies," says Zon. "Also, the more SETDBI was amplified, the worse the cancer, so we could also potentially use it as a diagnostic marker." Notably, SETDB1 is also over-expressed in ovarian, breast, and liver cancers.
For the second paper, Zon and 19 coauthors, including HHMI investigator Sean Morrison at the University of Michigan, examined the embryos of the zebrafish that were genetically modified to be prone to developing melanoma. The embryos appeared normal, but by analyzing their gene expression, Richard White, a postdoctoral researcher in Zon's lab, discovered a set of 127 genes that are mis-expressed in melanomas and that predict which fish will get melanoma.
Notably, these genes are important to a specialized stem/progenitor cell called the embryonic neural crest cell, which differentiates during development and gives rise to melanocytes, facial bones, and connective tissues. White showed that there were more of those cells than normal in the melanoma-prone embryos. "Essentially, these fish had extra stem cells," Zon says, "which perhaps makes the cancer more aggressive."
The team then screened 2,000 chemicals until they found one that perturbed the development of these neural crest cells. "We didn't have any idea what this molecule did," recalls Zon, but a database suggested that the molecule could block an enzyme called DHODH, or dihydroorotate dehydrogenase. The database also suggested that a drug used to treat rheumatoid arthritis drug, leflunomide, would have the same effect.
The scientists found that DHODH, an enzyme used to produce uridine (one of the RNA nucleic bases), is involved in transcribing DNA into RNA -- an essential step before the protein encoded by the gene can be manufactured. "We couldn't imagine how an enzyme important to every cell could be relevant to human melanoma or the development of the neural crest lineage," Zon says. "But we went further with a series of quite surprising experiments in zebrafish and human melanoma cell lines and discovered that leflunomide selectively blocks transcriptional elongation in melanocyte and neural crest genes. We don't know why inhibiting DHODH just stops these genes in their tracks, but that change in expression changes the cell's fate. The cell no longer thinks that it's the neural crest cell or a melanocyte. The drug takes the melanocyte out of the melanoma." But other cells and tissues were less affected by the drug.
After determining that leflunomide slowed the growth of tumors in mice engrafted with human melanoma, Zon's group combined it with a BRAF inhibitor made by Plexxikon. That drug is now in late stage clinical trials for metastatic melanoma. "In these trials, some tumors just melt away. But unfortunately the cancer usually returns after about six months," Zon says. "We thought combining that drug, which targets a specific oncogenic mutation, with leflunomide, which changes the cell's lineage, could have a beneficial effect."
It did, at least in mice. Compared to each drug alone, the combination led to a marked decrease in melanoma, and even with low doses of each drug the tumors went away completely in 40 percent of the mice. This drug combination may enter human clinical trials within a year, and it may be possible to use lower doses of each drug to decrease the risk of side effects and resistance.
Zon says the zebrafish is the ideal model for doing mechanistic studies that link genomics and biochemistry to understand how cancers occur in vivo and how to prevent them. "You need thousands of animals, and you would need an entire mouse facility to do what we can do with a few 50-gallon fish tanks." Also fish embryos grow externally, so researchers can plunk five embryos into each well of 96-well plates to screen thousands of chemicals to discover drug candidates.
Interestingly, some of genes that leflunomide pauses are those controlled by myc, a well known oncogene implicated in several cancer types. Recent work shows that myc controls transcription elongation in embryonic stem cells, and the zebrafish work now highlights myc's importance in melanoma as well. So as with the SETDB1 discovery, this finding may have relevance to other cancers -- and the zebrafish tank will be the perfect place to find out.
Source: ScienceDaily